Health coverage for millions at risk as tax credits expire
Between 22 and 24 million people will see premium increases, and 4 million are projected to lose coverage
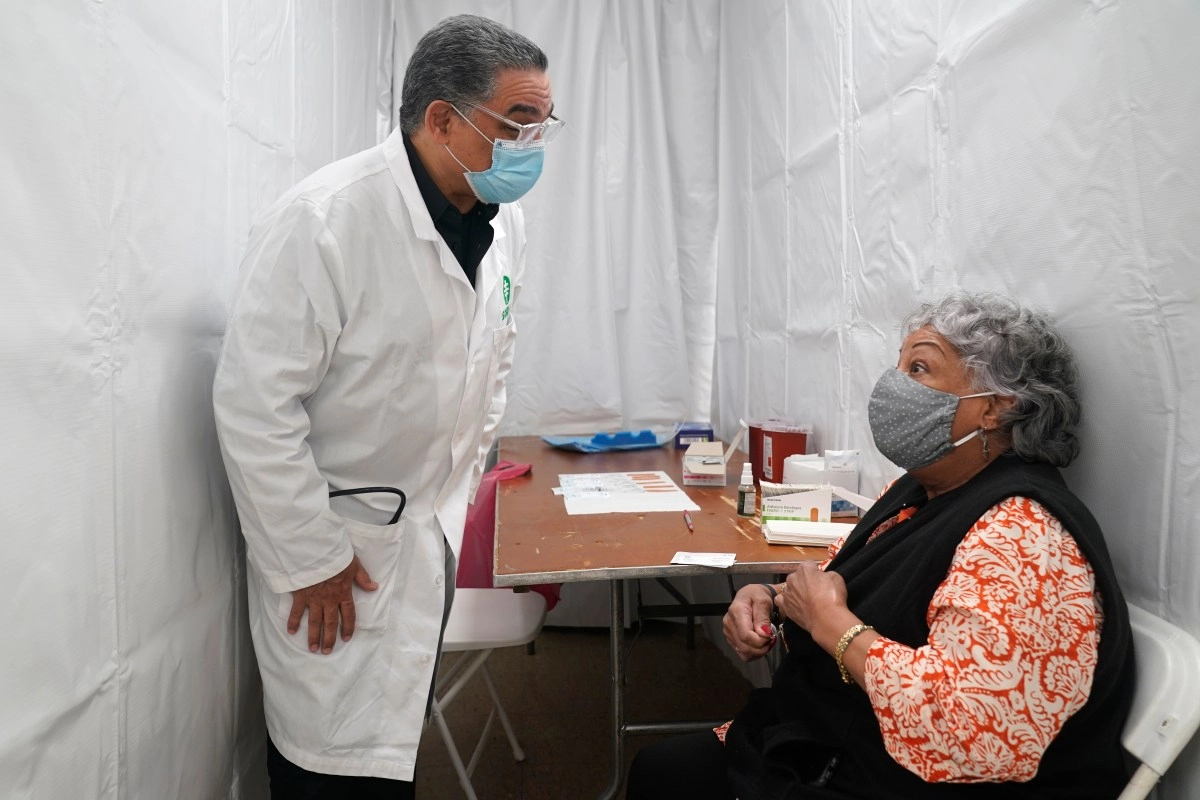
At the heart of the federal government shutdown, which began October 1, is skyrocketing health care costs.
Millions of Americans will get a shock this month when their monthly Affordable Care Act (ACA) premiums will nearly double because once enhanced premium tax credits expire at the end of the year, four million people will lose their health coverage immediately.
During the videoconference “As the government shutdown drags on, is a deal on health care costs possible?”, hosted by American Community Media (ACoM), Anthony Wright, executive director of Families USA, said that we are entering the second week of the government shutdown and just weeks away from November 1, the date when open enrollment begins for those who buy individual or family coverage.
“Half of us get coverage through our employers. Between a quarter and a third through public programs like Medicaid or Medicare, but the rest buy individual or family coverage, primarily through the marketplaces established by the Affordable Care Act.”
He said the vast majority of people signing up for this latest coverage are workers or small business owners, and they’re the ones who are going to see massive rate increases in the coming weeks as they head into open enrollment.
“Unless Congress takes action to extend these tax credits that help people afford coverage in every corner of this country,” he said.
He said that in the meantime, these people are opening their health plan letters with the news of a surprising increase, the result of new policy decisions this year, whether from the actions of the Trump administration or the health care cuts in the budget bill passed earlier this year.
“These increases are not inevitable. This is a political decision by Congress and this administration.After an election campaign promoting lower prices, President Trump and the Republican majority in Congress have failed to bring prices down as promised.”
In fact, he noted that when Republicans passed a tax package earlier this year extending tax cuts for the wealthy and large corporations, they repeatedly rejected several amendments that would have extended these tax credits that help low- and moderate-income people better afford their coverage.
He emphasized that time is ticking, and they have one last big opportunity, just before open enrollment starts on November 1.
He cited as an example the case of a 60-year-old person living in Maine who earns $65,000 a year and pays $460 a month for their coverage.
“Without the tax credit, that person goes from paying $460 a month to $1,400 a month, or more than $10,000 a year for be able to afford coverage.”
He said that on average, people will pay about $700 or $800 more a year, but especially if you are older, between 50 and 60 years old, the increase will be greater if you are in certain income groups or have a larger family.
In California’s case, those affected work in jobs that don’t offer health coverage and are disproportionately Latino.
“These are people who work in retail, restaurants, hospitality, and seasonal jobs, including perhaps some farmworkers. They are also gig workers, drivers for Uber, Lyft, and DoorDash.”
She also said there are many small business owners who will be affected, like a taco stand owner, a hair salon, or a beauty salon.
“Those are the kinds of people who sign up for coverage on healthcare.gov, on Covered California, and they are the ones who are directly affected by these massive increases, doubling or going beyond.”
Who will feel the biggest impact?
Jennifer Sullivan, director of health coverage access and leader of the “Beyond the Basics” project at the Center for Budget and Policy Priorities, said 93% of marketplace enrollees who receive a premium tax credit are at risk.
“These 22 million people are working people, but they have low incomes, less than four times the federal poverty level, and almost half below twice the poverty level, which is at about $32,000 a year.”
He said they are people who own small businesses or are self-employed, which represents one in four of the marketplace’s enrollees.
“We also have more than one in four of our health insurance marketplace enrollees who are young adults,people who have just graduated from high school or college, who have not yet found a job that offers insurance, but are too old to get it through their parents.”
She noted that at the other end of the age spectrum, we have people approaching the age of eligibility for Medicare.
“Nearly a quarter of health insurance marketplace enrollees are between 55 and 64, who already pay up to three times more for health coverage because of their age and are more likely to have acute health care needs.”
She said that people of color accounted for more than half of marketplace enrollees nationally in 2024, a 158% growth among Latinos and 186% for African Americans.
“The impact will be much greater in those communities.”
The biggest concern
Dr. Ashley Kirzinger, associate director of the program of KFF’s survey and public opinion research nonprofit, Health, Policy, Analysis, said that when they ask the public about their biggest financial worries, the cost of health care services and unexpected medical bills consistently rank at the top of that list, well above rent and mortgages, monthly utilities, and the cost of food and groceries.
“Nearly half of American adults say it’s difficult for them and their families to pay their health care costs, and one in four say a family member has struggled to pay for health care; and that's considering the premium tax credits."
She noted that African Americans and Hispanics and people with lower incomes are particularly likely to report trouble paying for health care.
"We conducted a survey before the shutdown to see if the public is aware of the expiration of the premium tax credits and found there has been a slight increase in public awareness."
However, she noted that only four in ten people overall say they've heard at least a little about it, and a similar share of those who buy their own coverage in the ACA health insurance marketplace.
"This means that six in ten people who buy their own coverage in the ACA health insurance marketplaces and will be affected by this have not yet heard much or anything about the expiration of these enhanced premium tax credits."


